Vision Assessment for people with Intellectual Disabilities
Image of a family: a middle aged, blonde lady with glasses is sharing a hug with a young man with Down syndrome, while a middle aged man with greying hair looks toward them affectionately.
If you know, care for, or work with, someone with intellectual disabilities, you may have wondered if it is possible for them to have their eye health and vision assessed, and if so, how would we accomplish this? maybe they are minimally verbal, or have a degree of echolalia (where a person repeats words immediately after hearing them), meaning that what they do say is not always reliable. In this article we’ll attempt to show how we can overcome those barriers.
People with intellectual disabilities should have their eye health and vision assessed, just like anyone else, but there can be barriers.
Preparation is key
Before we even get to the visit, we can help set the person up for success with a social story. Viewing a social story prior to visiting can be a fantastic way for the person to understand what will happen, ask questions, and manage anxieties. You can access our social story for adults here.
Let’s now move on to the eye examination itself.
History and entry questions
If you go along to get your eyes checked, the optometrist usually starts by asking some questions; they might ask you what prompted your visit, if you have ever had any problems with your eyes previously, if you have any medical conditions, and enquire about your family history.
For a lot of people with intellectual disability, this part can happen just the same, with a little support from a carer or family member. If the person is being accompanied by a carer, it can be helpful to gather some details from family members, since often they are the ones who are aware of childhood treatments and issues.
For some people, it can work better to provide this information before the visit, and this can be done via a brief phone consult in the days leading up to the appointment. At Special Eyes, we offer this option to all new patients.
Assessing visual acuity
Most people are familiar with the letter chart, as a standardised part of any vision assessment. It comes in various shapes and forms, and many are now digital, but the basic task remains the same: you are asked to read letters of decreasing size, until you reach a point where the letters are too small for you to see. Not everyone is able to read letters. Some people don’t know their letters, and obviously, this task is not appropriate or accessible for those who are non-speaking or minimally verbal. But there are many other ways to assess visual acuity.
Optometrist standing in front of a letter chart and pointing towards a line of letters using a red pointer on a stick.
Assessment of vision level actually begins from the moment we meet a patient. Observing how the person navigates the waiting room, and enters the testing room provides valuable information about their level of vision. If they stroll in, unaided, walk straight towards the chair, and take a seat, this tells us straight off that they have a reasonable level of vision. If they bump into the door frame on the way in, or are helped by a family member or carer, who is providing auditory description of their surroundings (“watch for the door” or “careful, there’s a chair there”) this provides an indication that their vision is reduced. In addition, there are a range of standardised vision tests we can use to further determine vision levels. Here are a few:
Cardiff Cards
Cardiff Cards visual acuity test. A red storage case with the Cardiff University logo in the background, in front of the box is a set of 3 grey cards, each with a picture of an apple, the apple is at the top on two of the card, and at the bottom on the third. At the very front of the image are two more cards, each displaying a picture of a boat; the boat image on the left is easy to see, but the one on the right is very faint and only just distinguishable.
Cardiff cards were developed for use with children and also adults with intellectual disabilities. The test uses the principle of ‘preferential looking’. As humans, we all choose to look towards something, in preference to nothing; when you are sitting in a waiting room with a tv mounted on the wall, if the tv is switched on, your attention will be drawn towards that, rather than sitting, staring at the blank wall surrounding it. So, Cardiff cards utilises this fact.
The person is shown a card which has a picture on it, the picture can be either at the top or the bottom of the card and the person presenting it, the examiner, does not know the location. The examiner gauges the person’s direction of gaze, and uses this to predict the location of the image, then checks the actual location to see if it matches.
Image of an optometrist holding up one of the Cardiff cards test cards, with an image of an apple, for a patient to view. She is looking towards the patient to judge their direction of gaze.
Lea Paddles
Lea paddles: 4 round targets with handles (the shape of a table tennis bat). The left one is plain grey, while the other 3 have vertical black and white stripes of varying widths.
Another assessment we can use is the Lea paddles. This is another ‘preferential looking’ test. The examiner holds up one plain grey, and one striped target, and monitors where the patient is looking. If the patient looks towards the strips, we can be fairly confident that they have seen them.
Image of an optometrist holding up the Lea paddles for a patient to view. The left paddles has black and white stripes, the right paddle is plain grey.
Determining if glasses are needed
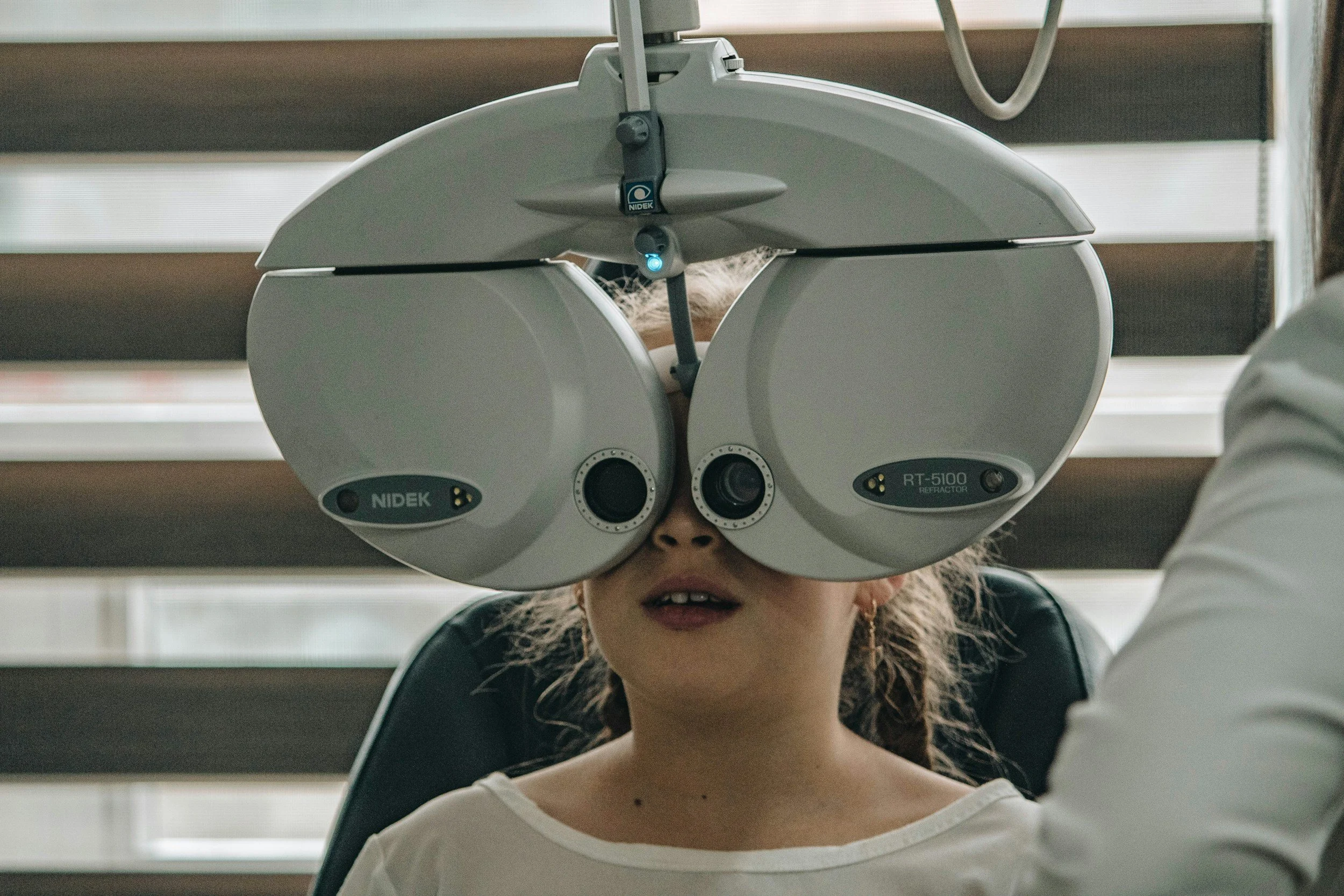
This is another core part of an eye and vision assessment. In many optometry practices, the optometrist will use something called a phoropter head to assess whether a person need glasses. Phoropter heads contain lots of different lenses. The patient looks through the eye holes, while the optometrist displays different strength lenses, to determine if they need glasses. There are usually a lot of questions, such as ‘better with one or two’ ‘better with, or without?'‘, and ‘which one is clearer, red or green?’.
Image of a child sitting behind a phoropter head: a large, oval shaped device, with two eye holes that the patient looks through.
This device, while convenient for the optometrist, tends to be rather confusing and intimidating for our patients with intellectual disabilities. We have found that many do better with the older style trial-frame glasses, pictured below.
A man wearing trial frame glasses with lenses in front of both eyes.
We also have many patients who really struggle tolerating anything on their face, and for these patients we can simply dispense with the frame, and hold the individual lenses up in front of their eyes.
So, once we have found a way to hold the lenses in front, there are options regarding how we measure the prescription. For some of our patients with intellectual disabilities, we can offer the same choices, but just with a bit more time, and clearer differences for them to differentiate. If this is too challenging, or for those with limited communcation, we can actually determine their prescription using a technique called retinoscopy. This involves shining a small light from a device called a retinoscope, in through their pupil. By assessing the movement of the light, we can determine whether a person needs glasses, and what prescription we need to put into these. The only thing our patient needs to do is have their eyes open - at least some of the time!
Optometrist performing retinoscopy: holding a retinoscope up to her eye with her right hand and directing the light from the device through a small lens, held in her left hand. This is how this assessment would look from a patient perspective.
Assessing eye health
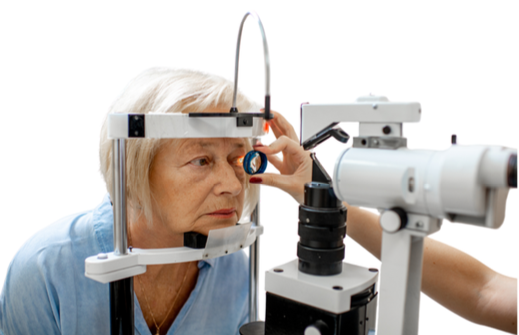
Assessing the health of the eyes is another core part of an eye test, and for many people with intellectual disabilities, they can still perform this assessment with just a little more guidance and support from the optometrist and their carers or family members. We typically use a device called a slit-lamp, pictured below.
Image of a lady, positioned with her chin resting on the chin rest of a slit-lamp. The optometrist is holding up a small lens close to one of her eyes and you can see the parts of the slit-lamp, which includes a bright light source and a binocular viewing system that the optometrist looks through.
Watching something you like on YouTube can also really help, so in our practice, we have an iPad that we can display on a tripod, which we position over the optometrist’s shoulder. The optometrist can view one eye, while the person watches their favourite You Tube videos with the other eye. It’s like being at the movies!
Sometimes we find that having a piece of medical equipment that close is just too tricky, and if that is the case, the optometrist can use a special headmounted device to have a look at the person’s eyes. We also have a hand held version of the slit lamp, which can be a bit less intimidating for some of our patients, see image below.
Optometrist using a hand held slit lamp device to view the front of the eye.
There are many other adjustments we can make to help support our patients with intellectual disabilities to access vision and eye health assessments. Providing equitable access to eye healthcare is really what we are all about here at Special Eyes, and we are always happy to work with out patients and those who support them to find ways to best accommodate their individual needs.
Want to learn more?
If you are supporting someone with an intellectual disability and would like to understand more about what and how they see, and / or make sure their eyes are healthy and establish if they need glasses, please reach out to us.
You can send an enquiry through our website, send us an email, or give us a call. Our reception is staffed between 10am and 2.30pm Mondays and Thursdays. We hope to hear from you soon.